
Applying Strength and Conditioning Principles to Cerebrovascular Accident (CVA) / Stroke Rehab
February 2025
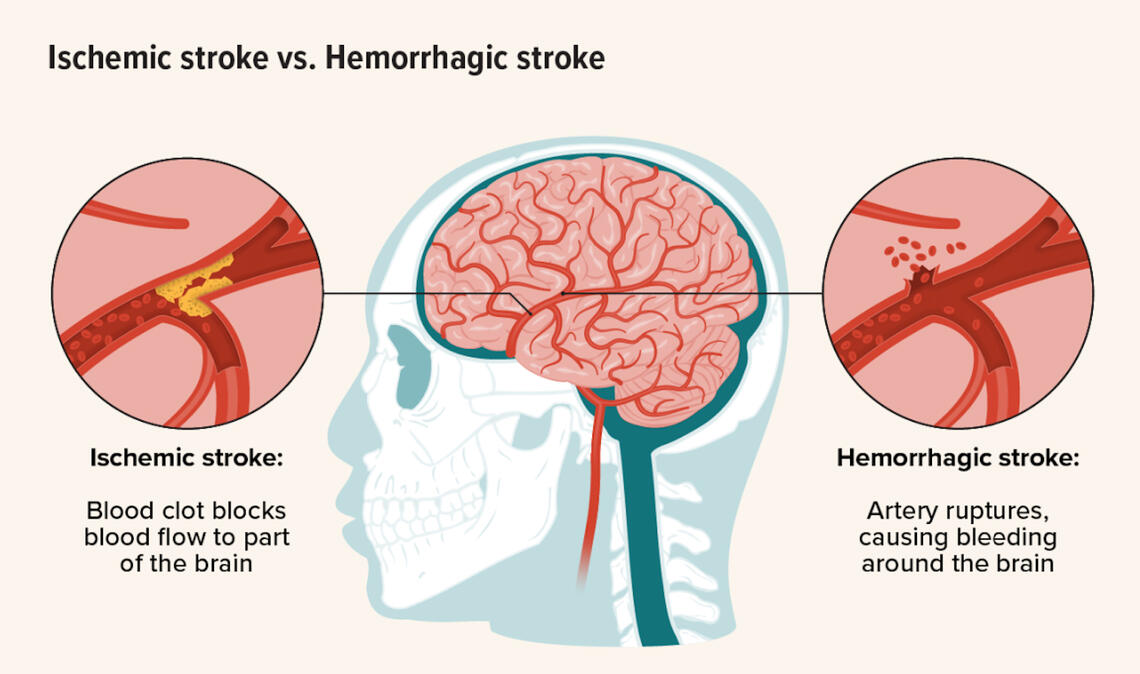
One common brain injury that physical therapists address is a cerebrovascular accident (CVA), commonly known as a stroke. Strokes are classified into two types: ischemic and hemorrhagic.1) Ischemic Stroke: This occurs due to a blockage in an artery, leading to reduced blood flow to brain tissue. As a result, the brain tissue is deprived of oxygen, potentially causing impaired function or tissue death2) Hemorrhagic Stroke: This results from the rupture of weakened blood vessels in the brain, leading to internal bleeding
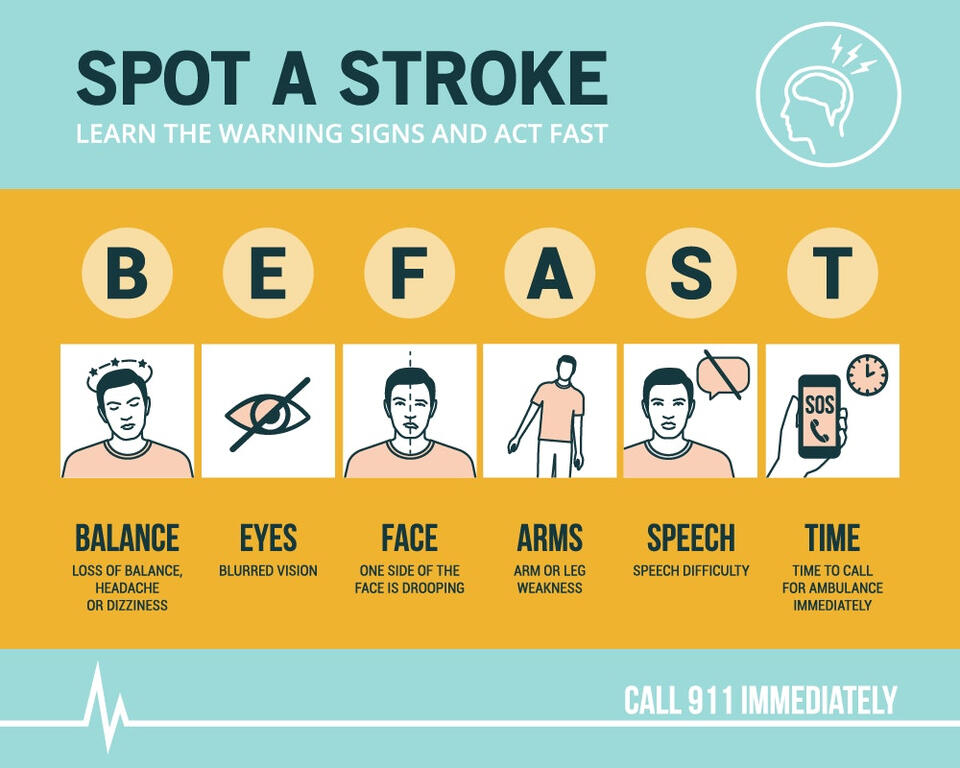
If someone is having a stroke, he or she may present with any of the following symptoms:B: Balance issues
E: Eye Changes
F: Face Drooping
A: Arm Weakness
S: Speech difficulty (slurring words, slow processing, confused speech, etc.)
T: TIME IS KEY (the faster you get help, the quicker the blockage or bleeding can be stopped to minimize damage)Remaining calm and understanding the necessary steps is crucial for providing quality care to someone experiencing an acute stroke.
The severity and deficits associated with a CVA depend on the specific location of the injury in the brain and the type of artery involved. For simplicity sake, we will break it down here:
Left Sided CVA
- Right sided weakness, atrophy, and hemiparesis- Speech and communication deficits (aphasias)
- Broca’s aphasia: impaired expressive speech, characterized by difficulty with word finding, fluent speech, and forming sentences
- Wernike’s aphasia: impaired receptive speech, resulting in poor comprehension; speech is effortless, but lacks meaningful content
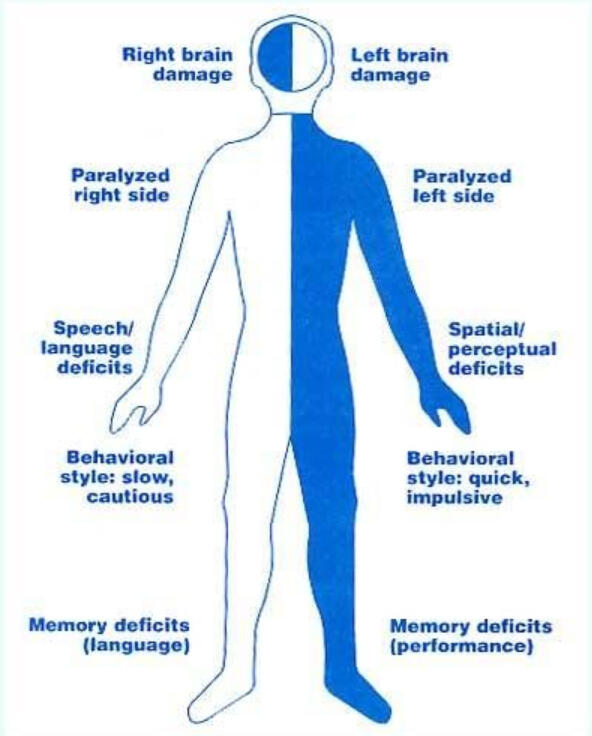
R Sided CVA
- Left sided weakness, atrophy, and hemiparesis- Left sided neglect: A lack of awareness or disregard for the left side of the body, affecting vision, touch, and spatial awareness
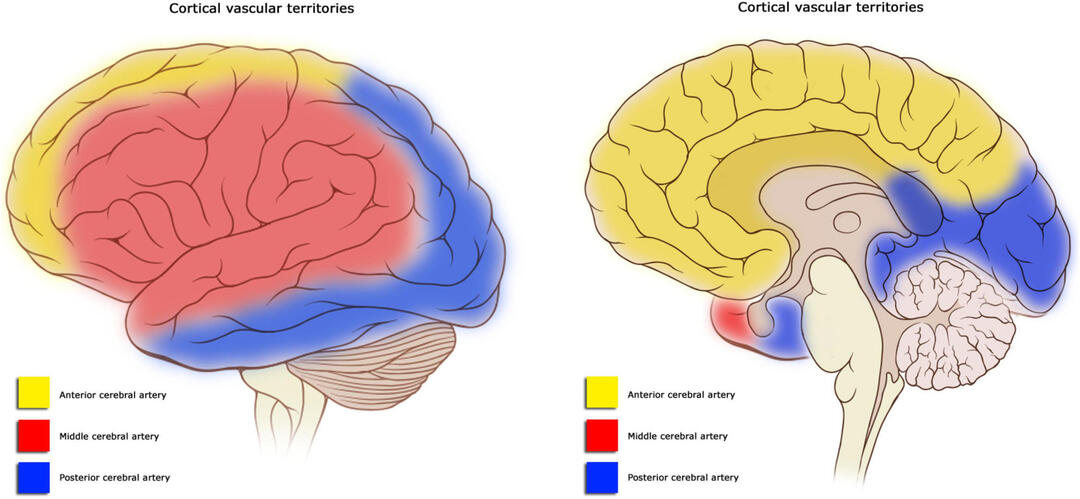
Three major arteries—the Anterior Cerebral Artery (ACA), Middle Cerebral Artery (MCA), and Posterior Cerebral Artery (PCA)—play a critical role in determining the deficits. Identifying the affected artery and understanding its vascular distribution (see diagram) can help predict the associated impairments.
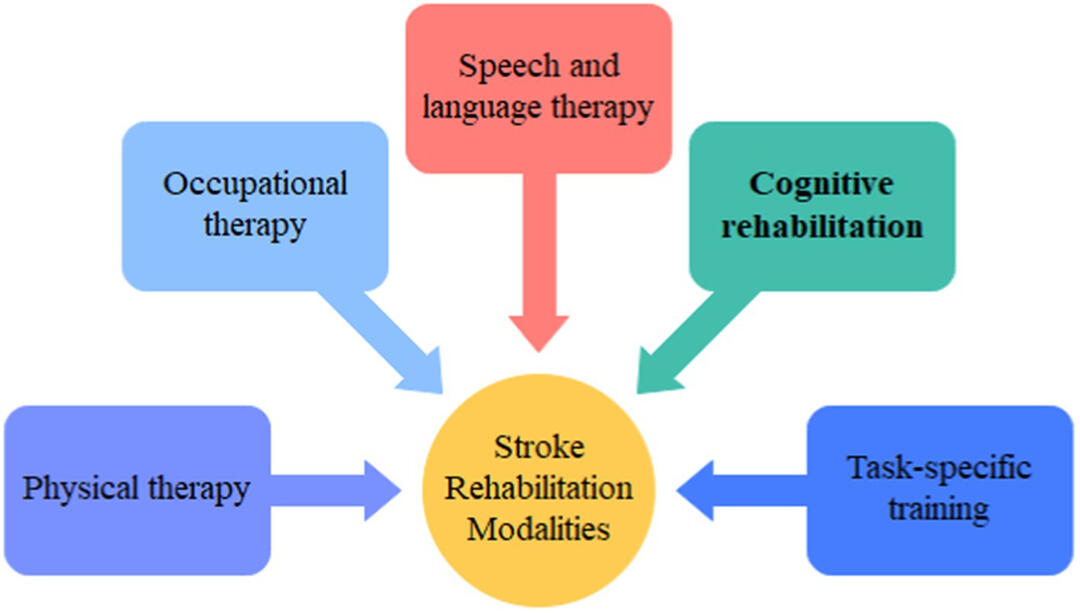
Once the individual is safe and stable, the recovery journey typically begins in an inpatient hospital setting and/or an acute rehabilitation facility, involving a team of physical therapists, occupational therapists, and speech therapists. From a physical therapy perspective, any central nervous system injury (affecting the brain or spinal cord) disrupts the signals sent to the upper and lower extremities, impairing overall function. The primary goal is to help patients regain safe mobility by restoring strength and usage in the affected side while addressing other related deficits, such as balance, coordination, and overall strength.
For the strength component, tapping into the scientific principles of strength training can serve as efficient and effective tools in patient recovery. From a strength and conditioning perspective, neural adaptations occur predominantly in the early stages of a resistance training program (1 day to 4 weeks), while muscle hypertrophy typically begins after approximately 10 weeks of consistent training (Haff & Triplett, 2021). Key neural adaptations include:- Increased rate of firing and synchronization of motor units, enhancing the signals sent to muscles- Heightened motor cortex activity, especially when force development increases or when learning new exercises- Enhanced connections between nerves and muscles, improving overall neuromuscular efficiency
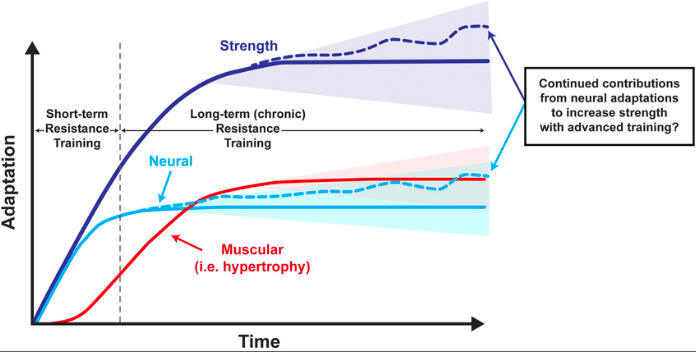

The brain is neuroplastic, meaning it has the ability to reorganize and rewire its neural connections in response to demands placed upon it. This capacity allows the brain to adapt and function in new ways after injury. Following a stroke, the nervous system represents a fertile ground for adaptive training responses (Sun et al., 2019). This process is comparable to the neural adaptations observed in novice lifters during the early stages of resistance training, often referred to as “newbie” or “beginner gains.”
Incorporating resistance training techniques and protocols can effectively prime the brain for neuroplastic changes in motor planning and coordination in patients recovering from a stroke. A 2019 study by Sun et al. demonstrated that progressive resistance training (> 70% of max. strength) decreased spasticity— characterized by high muscle tension and resistance to rapid stretching— and effectively increased muscle strength on the hemiparetic side, with large effect sizes (0.98; 95% CI, 0.67 to 1.29). Additionally, resistance training plays a vital role in brain health by stimulating the release of brain-derived neurotrophic factor (BDNF), a critical molecule for the growth, survival, and adaptation of the nervous system (Herold et al., 2019). The release of BDNF supports both structural and functional brain adaptations while enhancing cognitive functions.
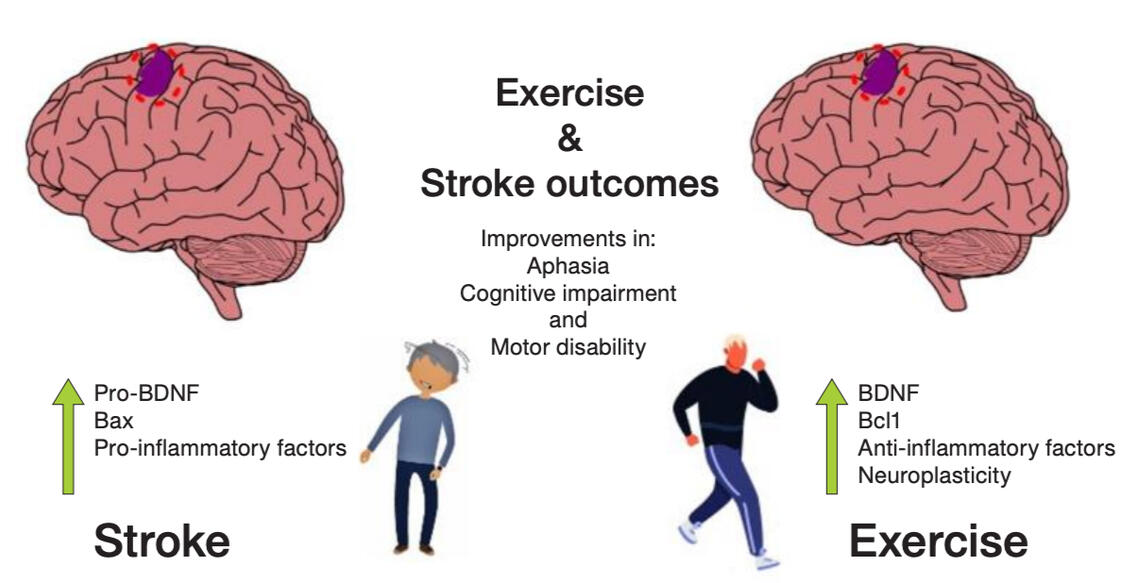
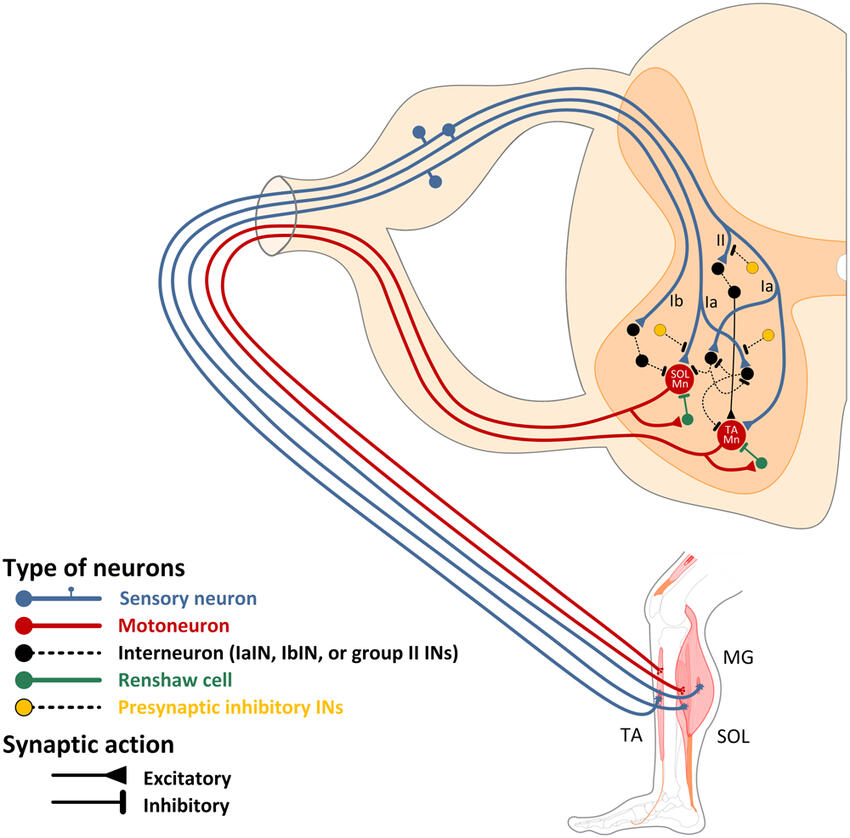
One underrated component of the aftermath of a stroke to the brain is the preservation of neural circuits below the site of injury, particularly within the spinal cord. Although compromised sensorimotor brain networks and descending regulation can lead to insufficient motor unit recruitment and reduced force production, the spinal neural connections between the upper and lower extremities generally remain intact (Sun et al., 2019). These spinal connections are essential for coordinating and smoothing interlimb movements during locomotion (Sun et al., 2019). In fact, this network allows animals to continue walking while recovering from an injured limb, so they do not get eaten by a predator. Harnessing the spinal cord’s capabilities, alongside strength and conditioning principles, can help reactivate the nervous system and significantly enhance the rehabilitation experience for stroke patients.
One fantastic tool involves the concept of cross education - overloading the uninvolved side to stimulate central neural factors that increase peak voluntary contraction on the untrained side (Haff and Triplet, 2021). When it is difficult to directly train the affected side, training the intact side can enhance neural excitability and muscle strength on the hemiparetic side by activating intact interlimb spinal neural pathways. Here are three key studies that highlight the effectiveness of cross-education:1) A meta-analysis of 96 cross-education training studies found a 29% strength gain on the untrained side in stroke patients, compared to an 18% increase in able-bodied young adults (Sun et al., 2019)2) In chronic stroke participants, Dragert and Zehr found 6 weeks of dorsiflexion (DF) training on the intact side led to a 34% increase in strength in the trained leg and a 31% increase in the untrained leg (Sun et al. 2019)3) Sun et al., 2018 reported that 5 weeks of training in chronic stroke patients resulted in a 42% increase in wrist extension force in the trained side and a 35% increase in the untrained side, with significant improvements in the hemiparetic upper extremity maintained for at least 5 weeks after training.
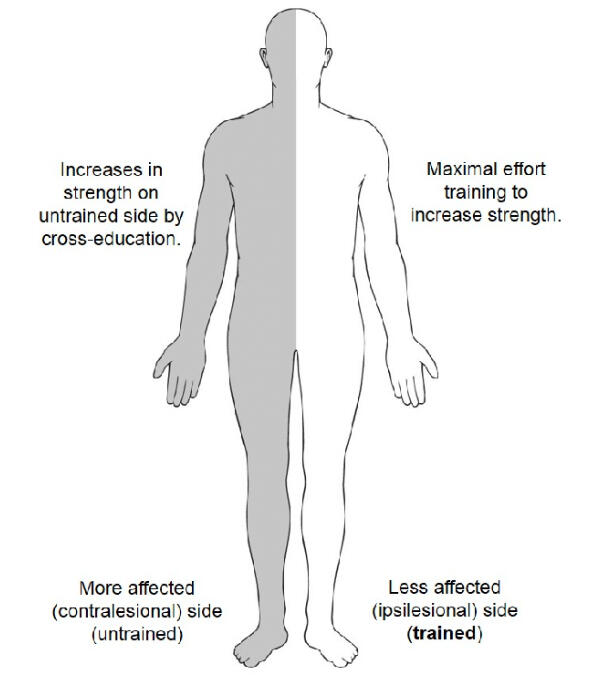
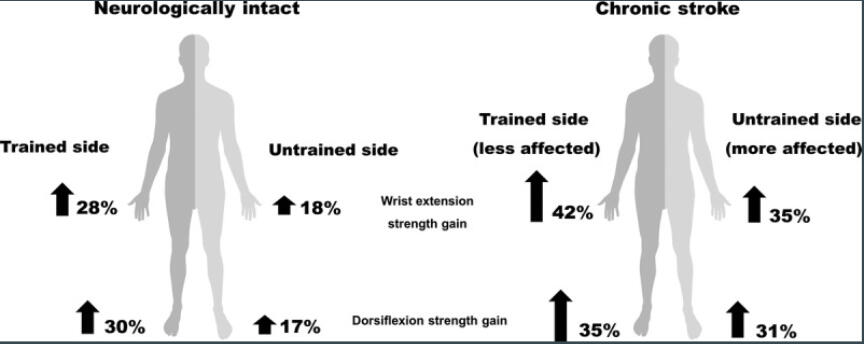
These neural adaptations and the percentage increase in strength on the hemiparetic limb indicate enhanced neuroplasticity in stroke participants compared to neurologically intact individuals (Sun et al., 2019). Once the affected side begins to initiate movement, the focus shifts to strengthening the affected side
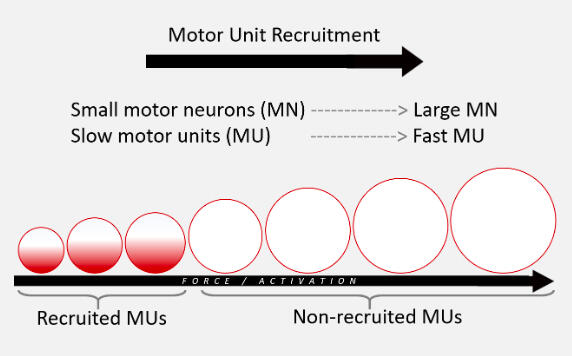
Another strength and conditioning concept beneficial for stroke patients is the size principle, which states that motor units are recruited in a specific order based on their size to produce high levels of force (Type I, Type IIa, Type IIx) (Haff and Triplet, 2021). To activate the nervous system and stimulate all muscle fibers, a strong overload stimulus is needed. One tactic would be an overcoming isometric, where bouts of effort at “maximum” intensity against immovable objects in order to increase neural drive and force production. This can be done through hands-on manual resistance, either on the uninvolved side (using cross education) or the involved side.For example, a sit-to-stand (STS) from a height the patient cannot fully rise from; although the patient may not complete the movement, maximal effort will lead to high motor unit recruitment that will lead to strength gains down the line. As long as safety is maintained, this type of training targets neural drive rather than the specific movement itself.
Another tactic would be post-activation potentiation (PAP), which states that previous strong contraction of a muscle can enhance subsequent contractions. A relatively heavy load stimulus generates significant nervous system excitation, which can be leveraged to improve performance Using manual resistance isometrics or manual eccentric resistance (muscle lengthening under tension) can prime the nervous system before performing more specific tasks that require strength, such as STS, stairs, and transfers.
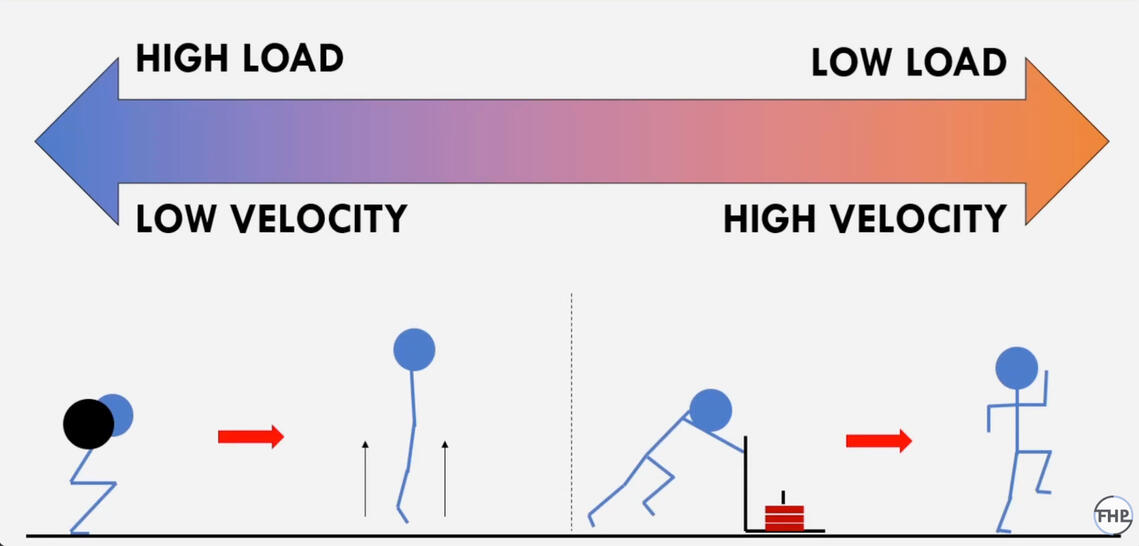
Why are rate of force development (strength) and power essential to CVA rehab?

Muscle power / explosive strength decline faster than muscle mass and strength; that is why they are more strongly associated with mortality and functional limitations (Alcazar et. al, 2020). Type II fibers (fast-twitch) decrease first with aging, followed by overall strength, and finally, muscle size.Eccentric strength – producing force while lengthening or going against gravity – also diminishes with age, contributing to an increased risk of falls and a significant decline in quality of life (QoL). When people fall, they usually fall down the stairs not up the stairs. For these patients, hemiparesis slow gait speed and double the physiological energy required for ambulation (Lee et al., 2020). For every 0.2 m/s increase in gait speed, there is a 38% reduction in the odds of demand for personal care” (Studenski, 2003). Among 292 men aged ≥ 60 yr, low muscle strength and slower gait speed correlated strongly with poor cognitive functioning (Sui et al., 2020).Lastly, incorporating strength training into CVA rehabilitation, in combination with cardiovascular training, offers the best potential outcomes for these patient populations.
The body and brain are capable of adapting and growing in response to the loads and demands placed upon them. After a stroke, a patient’s recovery journey provides a unique opportunity for neuroplasticity to take full effect. This is where applying a multidisciplinary approach—though it extends beyond its typical niche on the general population and sports or athletics – ensures the highest quality of care for patients during the darkest moments of their life.
